Master trauma-informed counseling: 67% of clients improve
Many therapists believe trauma-informed counseling guarantees better outcomes simply by adopting its principles. Reality proves far more nuanced. While trauma-informed approaches form essential foundations for ethical practice, effectiveness depends on precise application, cultural sensitivity, and advanced clinical skills. Research reveals significant evidence gaps alongside powerful trauma-focused interventions that deliver measurable results. This guide clarifies what works, examines critical limitations, and provides actionable strategies for mental health professionals seeking to elevate their trauma counseling expertise across diverse client populations.
Table of Contents
- Key takeaways
- Understanding trauma-informed counseling: principles and clinical foundation
- Evaluating effectiveness: evidence and limitations in trauma-informed practice
- Integrating cultural, gender, and ethical considerations in trauma-informed counseling
- Advanced training for trauma-informed counseling: skills for complex client support
- Explore advanced trauma-informed training with Mastering Conflict
- FAQ
Key Takeaways
| Point | Details |
|---|---|
| Ethical foundation | Trauma informed counseling is an ethical framework that informs practice rather than a standalone treatment, requiring careful application and cultural sensitivity. |
| Six core principles | The six core principles safety trustworthiness peer support collaboration empowerment and cultural relevance guide every client interaction and shape how you respond to resistance and interpret behavior. |
| Evidence is mixed | Broad trauma informed approaches show limited and bias prone evidence, while trauma focused therapies demonstrate stronger results for specific symptoms. |
| Targeted therapies outperform general care | For PTSD and related symptoms, trauma focused treatments such as cognitive processing therapy prolonged exposure and EMDR show consistent effectiveness and may be reinforced through blended care. |
Understanding trauma-informed counseling: principles and clinical foundation
Trauma-informed counseling recognizes how trauma impacts clients and integrates this knowledge throughout practice while actively preventing retraumatization. This approach differs fundamentally from trauma-specific therapies. Where trauma-focused treatments target specific symptoms using structured protocols, trauma-informed counseling creates a broader organizational and clinical culture that acknowledges trauma’s pervasive effects.
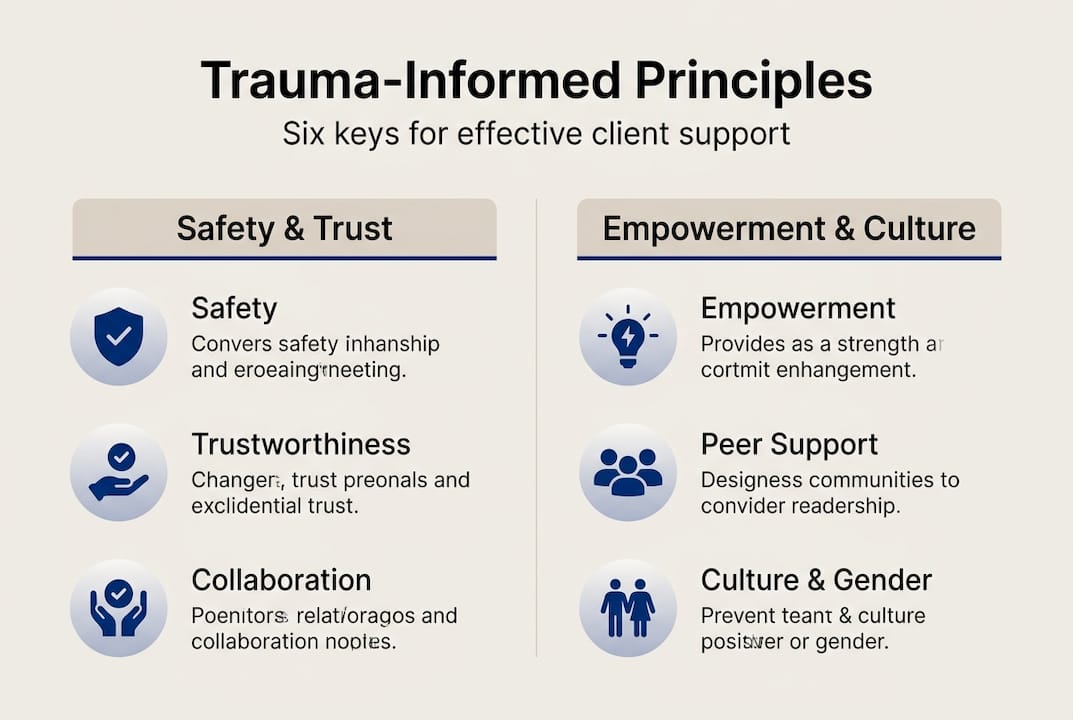
The framework rests on six core principles that guide every client interaction. Safety ensures physical and psychological security in therapeutic spaces. Trustworthiness demands transparency in clinical decisions and boundaries. Peer support recognizes the healing power of shared experiences and mutual aid. Collaboration distributes power between counselor and client, honoring client expertise in their own lives. Empowerment prioritizes skill building and client strengths rather than pathology. Cultural relevance requires counselors to address historical trauma, systemic oppression, and identity-based experiences that shape each client’s trauma response.
These principles transform how you structure sessions, respond to resistance, and conceptualize client behaviors. A client who misses appointments may be demonstrating trauma responses rather than lack of motivation. Sudden anger might reflect hypervigilance rather than defiance. Trauma-informed counseling trains you to recognize these patterns without labeling them as treatment resistance.
Pro Tip: Create a visual checklist of the six principles and review it before each session during your first month of implementation. This builds automatic trauma-informed thinking patterns that become second nature over time.
Every therapeutic interaction becomes an opportunity to model safety and collaboration. You explain treatment rationales clearly, invite client feedback on session structure, and acknowledge power differentials inherent in the counselor role. This foundation supports all subsequent interventions, whether you’re addressing depression, relationship conflict, or substance use. Trauma-informed counseling isn’t a standalone treatment but rather the ethical bedrock upon which effective therapy stands.
Evaluating effectiveness: evidence and limitations in trauma-informed practice
Research on trauma-informed counseling reveals a complex evidence landscape that demands careful interpretation. Broad trauma-informed counseling shows limited effectiveness evidence across diverse outcomes, with studies demonstrating high risk of bias. This doesn’t mean the approach fails, but rather that rigorous research hasn’t yet confirmed its impact as definitively as clinicians might hope.
Contrast this with trauma-focused therapies. Blended care approaches combining face-to-face and digital interventions show large effect sizes for PTSD symptom reduction. Cognitive processing therapy, prolonged exposure, and EMDR demonstrate consistent effectiveness when applied to specific trauma presentations. The distinction matters critically for your practice decisions.
| Therapy type | Primary focus | Evidence strength | Best application |
|---|---|---|---|
| Trauma-informed counseling | Organizational culture, safety principles | Moderate, high bias risk | Universal foundation for all clients |
| Trauma-focused CBT | Specific PTSD symptoms, trauma memories | Strong, large effect sizes | Diagnosed PTSD, recent trauma |
| EMDR | Memory reprocessing, bilateral stimulation | Strong for PTSD | Single-incident trauma, PTSD |
| Somatic experiencing | Body-based trauma release | Emerging evidence | Complex trauma, dissociation |
Critical voices raise important cautions. Some researchers argue trauma-informed care risks pathologizing normal stress responses and reducing client agency by framing all difficulties through a trauma lens. Critics emphasize that overgeneralizing trauma concepts can lead to harm, particularly when cultural contexts are ignored or when trauma frameworks become politically charged rather than clinically precise.
“The trauma-informed approach must balance recognition of trauma’s real impacts with respect for client autonomy and cultural meaning-making. Overemphasis on vulnerability can inadvertently disempower the very clients we aim to support.”
These limitations don’t invalidate trauma-informed principles but demand thoughtful application. You must distinguish between creating trauma-aware environments and claiming trauma-informed counseling alone treats specific trauma disorders. When clients present with PTSD symptoms, understanding the relationship between trauma responses like anger and underlying PTSD guides you toward evidence-based trauma-focused interventions rather than relying solely on general trauma-informed principles.
The evidence suggests a layered approach. Build your practice on trauma-informed foundations while deploying trauma-focused therapies when clients present with diagnosable trauma-related conditions. This integration honors both the ethical imperative of trauma awareness and the clinical necessity of targeted, effective treatment.
Integrating cultural, gender, and ethical considerations in trauma-informed counseling
Cultural humility transforms trauma-informed counseling from a universal framework into a responsive, individualized practice. Integrating cultural perspectives and gender-sensitive approaches, such as trauma-focused cognitive behavioral therapy adapted for sexual violence survivors, dramatically improves safety and collaborative engagement. You cannot apply trauma-informed principles effectively without addressing how culture shapes trauma experiences, expressions, and healing pathways.

Historical trauma compounds individual experiences for many populations. Black clients may carry intergenerational trauma from slavery, segregation, and ongoing systemic racism. Indigenous clients face trauma rooted in colonization and forced assimilation. LGBTQ+ individuals navigate minority stress and discrimination trauma. Gender-based violence survivors require approaches that recognize power dynamics and societal attitudes toward sexual assault. Each context demands specific adaptations to standard trauma-informed practices.
Implementing culturally responsive trauma counseling requires concrete actions:
- Acknowledge your own cultural background and biases through ongoing self-reflection and supervision
- Learn specific historical and contemporary trauma contexts affecting your client populations
- Adapt language, metaphors, and therapeutic activities to align with client cultural frameworks
- Collaborate with cultural brokers, community leaders, and indigenous healers when appropriate
- Recognize that Western psychological concepts may not translate across all cultural contexts
Gender considerations extend beyond binary categories. Trauma responses vary across gender identities, with some research showing differences in symptom presentation, help-seeking behaviors, and treatment engagement. Women survivors of interpersonal violence may prioritize safety planning and empowerment, while men may struggle with shame and societal expectations around victimhood. Transgender and nonbinary clients face unique trauma risks related to discrimination and violence.
Cultural considerations in couples therapy apply equally to individual trauma work, requiring you to understand how cultural norms around emotion expression, family loyalty, and help-seeking influence treatment engagement. When working with Black families, recognize the protective factors of community, spirituality, and resilience alongside trauma vulnerabilities.
Pro Tip: During intake, explicitly ask clients how their cultural background and identity influence their comfort in therapy. This conversation signals your openness and provides crucial information for tailoring your trauma-informed approach.
Ethical challenges emerge when trauma-informed principles conflict with client autonomy. Some clients reject trauma frameworks for their experiences, preferring alternative explanations rooted in spiritual beliefs, systemic analysis, or personal meaning-making. Imposing trauma interpretations violates the collaboration principle central to trauma-informed care. Your role involves offering trauma perspectives while respecting client authority over their own narrative.
Balance requires constant calibration. You must remain alert to trauma indicators without pathologizing every client struggle. You create safety without fostering dependency. You acknowledge vulnerability while reinforcing strength and agency. This nuanced practice develops through experience, supervision, and genuine commitment to cultural humility rather than cultural competence claims.
Advanced training for trauma-informed counseling: skills for complex client support
Advanced trauma counseling demands specialized skills beyond foundational principles. Training should emphasize biopsychosocial trauma understanding, somatic interventions for dissociation and complex PTSD, and therapeutic alliance rupture management. These competencies separate adequate trauma-informed practice from excellence in supporting clients with complex presentations.
Biopsychosocial trauma assessment integrates biological stress responses, psychological coping mechanisms, and social context factors. You learn to recognize how trauma alters nervous system functioning, creating hyperarousal or hypoarousal states that clients cannot simply “think” their way out of. Polyvagal theory explains why some clients shut down while others become combative when triggered. This knowledge prevents misinterpreting trauma responses as resistance or personality pathology.
Somatic approaches address trauma stored in the body rather than solely in conscious memory. Clients with complex PTSD and dissociation often benefit more from body-based interventions than traditional talk therapy alone. Techniques include:
- Grounding exercises that anchor clients in present moment sensory experience
- Progressive muscle relaxation to release chronic tension patterns
- Breathwork that regulates autonomic nervous system activation
- Movement practices that help clients reconnect with physical sensations safely
- Pendulation between trauma activation and resourcing to build tolerance
Therapeutic alliance ruptures occur frequently in trauma work. Clients may suddenly withdraw, become hostile, or miss sessions after particularly vulnerable disclosures. Rather than viewing these as treatment failures, advanced practitioners recognize ruptures as opportunities for repair that mirror and heal relational trauma patterns. You acknowledge the rupture directly, explore what triggered it without defensiveness, and collaborate on repairing the connection. This process often proves more healing than sessions without rupture.
Conflict management methods apply directly to alliance rupture repair, as do broader conflict management skills that help clients navigate relationships outside therapy. When you model healthy conflict repair in the therapeutic relationship, clients internalize new relational possibilities.
Pro Tip: After any session where you sense disconnection or tension, send a brief follow-up message acknowledging the difficulty and reaffirming your commitment to the therapeutic relationship. This proactive repair prevents dropout and models secure attachment.
Comparing trauma-focused modalities helps you match interventions to client needs:
| Modality | Core mechanism | Session structure | Best for | Avoid when |
|---|---|---|---|---|
| Prolonged exposure | Habituation through repeated trauma narrative | 90-minute sessions, homework | Single-event PTSD, avoidance | Active substance use, severe dissociation |
| Cognitive processing therapy | Cognitive restructuring of trauma meanings | 60-minute sessions, worksheets | Self-blame, guilt, chronic PTSD | Cognitive impairment |
| EMDR | Bilateral stimulation during memory recall | 90-minute sessions, 8-phase protocol | All PTSD types, recent or past | Unstable clients, uncontrolled environments |
| Somatic experiencing | Body sensation tracking and release | 60-minute sessions, gentle pacing | Complex trauma, developmental trauma | Clients uncomfortable with body focus |
Advanced training also addresses vicarious trauma and counselor self-care. Regular supervision, peer consultation, and personal therapy help you process the emotional weight of trauma work. You cannot pour from an empty cup, and maintaining your own nervous system regulation enables you to co-regulate with dysregulated clients.
Continuing education should include live supervision with complex cases rather than only didactic learning. Watching experienced trauma counselors navigate difficult moments, receiving real-time feedback on your interventions, and practicing skills in role-plays builds competence that reading alone cannot achieve. Seek training that includes diverse client populations and presentations rather than one-size-fits-all approaches.
Explore advanced trauma-informed training with Mastering Conflict
Deepening your trauma-informed counseling expertise requires ongoing education and practical application. Mastering Conflict offers specialized courses designed specifically for mental health professionals seeking to enhance their trauma counseling skills with diverse client populations. These programs integrate evidence-based practices with cultural sensitivity and advanced clinical techniques covered throughout this guide.
Understanding the distinction between coaching and therapy clarifies your professional role when working with trauma survivors, ensuring you provide appropriate interventions within your scope of practice. For practitioners expanding access to underserved populations, teletherapy counseling services offer flexible delivery models that maintain trauma-informed principles while reaching clients who face geographic or mobility barriers. Investing in your professional development directly translates to improved client outcomes and greater confidence managing complex trauma presentations.
FAQ
What is trauma-informed counseling and how is it different from trauma-focused therapy?
Trauma-informed counseling creates organizational cultures and clinical practices that recognize trauma’s widespread impact, prioritize safety, and avoid retraumatization across all clients regardless of presenting concerns. Trauma-focused therapy targets specific trauma symptoms using structured, evidence-based treatments like prolonged exposure or EMDR for clients with diagnosed trauma-related disorders. Think of trauma-informed counseling as the foundation and trauma-focused therapy as the specialized intervention built upon it.
How can counselors address cultural diversity effectively in trauma-informed care?
Incorporate cultural humility by continuously examining your own biases and learning about historical trauma contexts affecting specific populations. Recognize how gender, race, ethnicity, sexual orientation, and other identity factors shape trauma experiences and healing pathways. Adapt therapeutic language, activities, and goals to align with client cultural frameworks rather than imposing Western psychological concepts. Explore cultural considerations that enhance engagement and prevent inadvertent retraumatization.
What advanced skills should therapists develop for complex trauma cases?
Focus on somatic techniques that address trauma stored in the body, including grounding exercises and nervous system regulation strategies for clients with dissociation. Master therapeutic alliance rupture recognition and repair, as these moments often replicate and heal relational trauma patterns. Develop biopsychosocial trauma understanding that integrates biological stress responses with psychological and social factors. Learn conflict management methods that support both alliance repair and client relationship skills outside therapy.
When should counselors refer clients to trauma-focused therapy specialists?
Refer when clients present with diagnosed PTSD, complex PTSD, or dissociative disorders requiring specialized interventions beyond general trauma-informed counseling. Consider referral if you lack specific training in evidence-based trauma treatments like prolonged exposure, cognitive processing therapy, or EMDR. Clients with severe dissociation, active suicidality related to trauma, or comorbid conditions requiring integrated treatment may benefit from specialists with advanced trauma training and appropriate supervision structures.
Recommended
- Mental Health Counseling Explained: Impactful Solutions – Mastering Conflict
- Counseling for Black Families: Culturally Centered Healing – Mastering Conflict
- Family Counseling Benefits: Support, Healing, and Connection 2025 – Mastering Conflict
- Conflict Management Method: Enhancing Therapy Outcomes – Mastering Conflict
- Couples Therapy Through the Lens of CBT: Strengthening Relationships – MindWell

